- Call Us: 9916809215
- Email Us: nithinr2711@gmail.com
Kidney Care Clinic
About Us
5+
Years of Experience
10K+
CKD Cases Managed
5K+
Uncontrolled Hypertension Cases Managed
25K+
Happy Patients
Our Specialization
Our Healthcare Services
Advanced, patient-focused nephrology treatments for lasting wellness
Dr. Nithin R
About Doctor
 (1).png)
- MBBS, MD Internal Medicine, DM Nephrology
- 5.0 Years Of Experience
- Licence No. 90829-KMC
- Video Call
- In person
Media Pictures

Frequently Asked Questions
Need Answers? Find them here...
Dr. Nithin R is a skilled and dedicated Nephrologist with over three years of specialized experience in managing a wide range of kidney-related conditions. He earned his DM in Nephrology from St. John’s Medical College Hospital, Bengaluru, where he conducted original research on caregiver burden in continuous ambulatory peritoneal dialysis. His expertise spans Chronic Kidney Disease (CKD) and End-Stage Kidney Disease (ESKD) care, dialysis management, interventional nephrology, and kidney transplantation, with a focus on patient comfort and personalized treatment plans.
Dr. Nithin R ensures quality care by combining evidence-based medicine with a compassionate, patient-centered approach. He offers comprehensive expertise in areas such as interventional nephrology, dialysis planning, and transplant evaluations. Actively engaged in academic research and presentations at national conferences, he stays updated with the latest advancements in nephrology. Dr. Nithin’s commitment to personalized treatment plans aims to enhance kidney function and prevent disease progression, significantly improving patients' quality of life.
Chronic Kidney Disease (CKD) is a condition characterized by gradual loss of kidney function over time. It manifests in stages and can progress to End-Stage Kidney Disease (ESKD) if unmanaged. Management includes controlling blood pressure, managing diabetes, dietary modifications, and medication to slow disease progression. Regular monitoring and follow-up with a nephrologist are crucial for effective CKD management and preventing further complications.
End-Stage Kidney Disease (ESKD) occurs when kidneys lose nearly all capacity to function effectively, typically at less than 15% of normal kidney function. Treatment options include dialysis, either hemodialysis or peritoneal dialysis, and kidney transplantation. A renal transplant specialist can evaluate the patient for transplantation viability while planning dialysis is essential for those not eligible or waiting for a transplant.
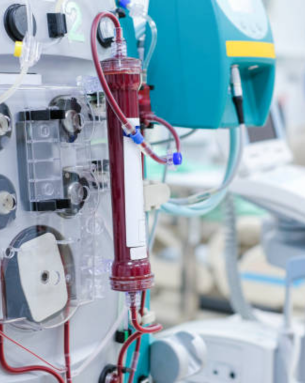
Dialysis planning for CKD patients involves evaluating when dialysis should begin, which type of dialysis is best suited (hemodialysis or peritoneal dialysis), and creating a vascular access point if needed. Interventional nephrology may be involved to assess and prepare arteriovenous fistulas or grafts. Regular assessment of kidney function and symptoms guides the timing for initiating dialysis to maintain quality of life.
Interventional nephrology includes procedures and techniques to improve dialysis access and manage kidney-related conditions. It involves creating, maintaining, and managing vascular access points like arteriovenous fistulas or grafts for dialysis patients. Interventional nephrologists also handle procedures such as biopsies and catheter placements, ensuring efficient dialysis and better outcomes for CKD and ESKD patients.
Pre-kidney transplant evaluation assesses a patient's medical condition, compatibility, and readiness for transplantation. It involves comprehensive tests to determine kidney function, donor compatibility, and other health evaluations. Post-kidney transplant evaluation focuses on monitoring the new kidney's function, preventing rejection, and managing medications to ensure graft longevity and patient health, with regular follow-ups and adjustments.
Hypertension and diabetic kidney disease management involves regulating blood pressure and blood sugar levels to protect kidney health. Medications such as ACE inhibitors or ARBs are employed, along with lifestyle modifications like diet change and physical activity. Monitoring kidney function and ensuring diabetic control are vital to prevent progression towards CKD, necessitating regular nephrologist follow-ups.
Acute kidney injury (AKI) is a sudden decline in kidney function often due to injury, infection, or medication. Management involves identifying and treating the underlying cause, maintaining fluid balance, and monitoring electrolytes. In severe cases, temporary dialysis may be needed. Preventive measures and early intervention are crucial in preventing further complications and promoting kidney recovery.
Uncontrolled hypertension can exacerbate kidney disease and require comprehensive management involving medication adjustments, lifestyle changes, and routine monitoring. Techniques include optimizing antihypertensive therapy, dietary salt reduction, and addressing underlying causes. Nephrologists play a critical role in evaluating secondary causes of hypertension related to kidney disease, promoting effective blood pressure control to prevent further kidney damage.
Preventive nephrology focuses on preventing kidney disease progression and its complications by managing risk factors and educating patients. This involves early intervention in conditions like hypertension and diabetes, regular monitoring of kidney function, and promoting healthy lifestyle choices. Preventive nephrology aims to delay or avert CKD development, improving patients' quality of life and reducing the burden on health systems.
Nephrotic Syndrome is marked by excessive protein loss in urine and can be due to various kidney disorders. Treatment focuses on addressing the underlying cause, reducing symptoms, and preventing complications. This includes corticosteroids or immunosuppressive medications, blood pressure control, reducing cholesterol levels, and dietary adjustments. Nephrologists provide tailored treatment plans to manage symptoms effectively and monitor for progression to CKD.

.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)